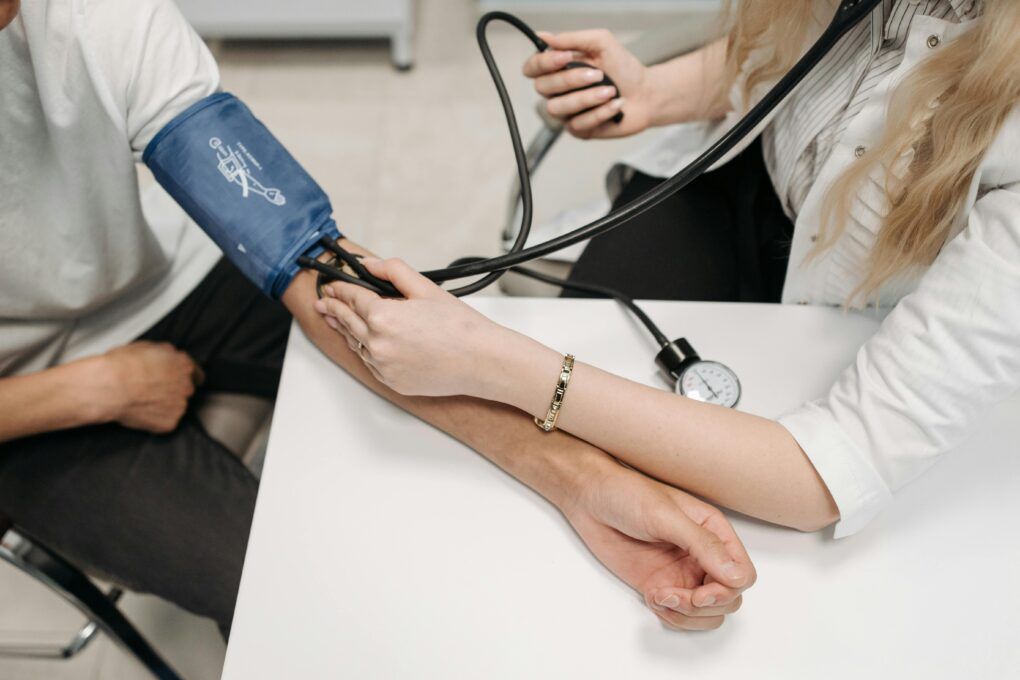
As part of our #MyGPandMe campaign we are campaigning for quality and accessible Annual Health Checks for people with learning disabilities. Use our free resources and tell us how your GP practice is helping make things better for you.
We think it’s wrong that people with learning disabilities die at least 20 years’ younger than the general population, and often from preventable or treatable health issues (LeDeR 2023) that could be picked up by a good quality Annual Health Check.
Early and preventable deaths
We know that an Annual Health Check is fair healthcare and it’s a chance to keep track of someone’s health at least once a year, if they are over 14 and on their GP Learning Disability Register.
But around 75% of people are not enrolled on the Learning Disability Register and often struggle to convince their GP and practice staff to add them to it (WEC). Our friends at Mencap are campaigning to make this better.
We are also shocked that the government has stopped asking GPs to prioritise Annual Health Checks, even though they have recently announced their commitment to reducing health inequalities.
We need to ensure that people with learning disabilities and autistic people are not forgotten. Use and share our resources and tell us how your GP practice is helping make things accessible.
Latest health resources
-
 Guide21st November 2025
Guide21st November 2025For Health Professionals: GP Quick Guides
-
 Guide20th November 2025
Guide20th November 2025For Health Professionals: GP guide to Annual Health Checks
-
 Template19th November 2025
Template19th November 2025Tips to help me at the doctors